The Things People say

Raising a Child with Type 1
When a child has Type 1 diabetes, people don’t just offer support.
They offer opinions.
Advice.
Observations.
Comparisons.
Most of it is well-intentioned.
Some of it is uninformed.
All of it reminds you that chronic illness invites commentary.
“At Least It’s Manageable.”
Yes.
It is manageable.
We are grateful it is manageable.
But manageable doesn’t mean simple.
It doesn’t mean light.
It doesn’t mean we forget about it for hours at a time.
It means we work at it daily.
Quietly.
Consistently.
Without applause.
“She Doesn’t Look Sick.”
She isn’t sick.
That’s the thing.
Type 1 isn’t a flu you recover from.
It’s a condition you carry invisibly.
She looks healthy because she works hard at staying that way.
Because we work hard at staying that way.
Looking “normal” is not the absence of effort.
It’s the result of it.
“Can’t She Just Avoid Sugar?”
Type 1 diabetes is not caused by eating sugar.
And it’s not cured by avoiding it.
Her pancreas does not produce insulin.
That’s it.
It’s autoimmune.
It’s biological.
It’s not behavioural.
We count carbs in broccoli and strawberries the same way we count them in cake.
Food isn’t the villain.
Insulin is the tool.
“You’re So Calm About It.”
We are calm about it.
Because she needs us to be.
But calm doesn’t mean untouched.
It means steady.
It means choosing composure.
It means processing the fear privately, so she doesn’t carry it publicly
“There Are Worse Things.”
There are.
Always.
Perspective matters.
Gratitude matters.
But comparison doesn’t erase reality.
This is still her reality.
And it deserves care without minimisation.
The Truth Beneath the Comments
Most people don’t mean harm.
They’re trying to place something unfamiliar into a familiar box.
But Type 1 doesn’t fit neatly.
It’s not cured by diet.
It’s not outgrown.
It’s not occasional.
It’s constant.
What Actually Helps
“What do you need?”
“How’s she going?”
“Is there anything I should know?”
And sometimes, simply —
“I can’t imagine that’s easy.”
Those words hold space instead of filling it.
And space is far more supportive than advice.
Teaching Grace
I’m teaching her something through all of this.
How to correct misinformation kindly.
How to explain without defensiveness.
How to advocate without anger.
How to hold her reality confidently.
Because people will always say things.
And she will always be more than the condition they’re trying to understand.
Travel, Heat & Carry - On Bags

Raising a Child with Type 1 –
We still travel.
That’s the first thing I decided after diagnosis.
Diabetes would come with us.
It wouldn’t stop us.
But it does mean we pack differently.
The Medical Carry-On
Before Type 1, travel packing was about outfits and toiletries.
Now, it begins with a medical inventory.
Insulin (double what we need).
Backup insulin.
Pump supplies.
Spare pods or infusion sets.
CGM sensors.
Transmitters and charging cables.
Glucose meter and strips.
Lancets.
Hypo treatments.
Glucagon.
Ketone strips.
Adhesives.
Overpatches.
It will mean a Medical letter for airport security.
And then — backup for the backup.
It will all go in carry-on.
Always.
Because luggage can get lost.
Insulin cannot.
Heat Changes Everything
We think about temperature now.
Insulin doesn’t like heat.
Airports, tarmacs, European summers,
Australian beach days — all require planning.
Cooling packs.
Shaded storage.
Never leaving supplies in the car.
Watching hotel room air-conditioning.
There’s a quiet awareness that something as ordinary as a hot day can compromise something as critical as medication.
So, we plan.
Again.
Airport Security
There’s going to be a new conversation at security.
“Yes, it’s medical.”
“No, it can’t go through the scanner.”
“Yes, she’s wearing a device.”
We will become practiced at calm explanation.
I hope Most staff are kind.
And Some won’t fully understand.
But we are learning to advocate — not loudly — just clearly.
It becomes second nature.
The Myth of “Relaxing”
Holidays still mean joy.
Swimming.
Late nights.
Different food.
Different time zones.
Gelato in Rome.
Chocolate croissants in Paris.
But they also mean:
Different carb counts.
Different activity levels.
Late-night corrections.
Adjusted basal rates.
Monitoring through jet lag.
You can relax — just not completely.
There’s always a layer of awareness beneath the enjoyment.
The Courage to Keep Going
Some might ask why bother.
Why not just stay close to home?
Because she deserves a full life.
A life bigger than diabetes.
She deserves travel stories.
Passport stamps.
Hotel breakfasts.
Beach days.
City nights.
Adventure.
So we pack more.
We think ahead.
We calculate across time zones.
We carry the pharmacy in our backpacks.
And we go anyway.
Living, Not Waiting
Chronic illness can quietly shrink a world if you let it.
I refuse.
We don’t wait for perfect conditions.
We don’t wait for better technology.
We don’t wait for a cure before we live.
We travel.
We plan.
We adapt.
Diabetes comes with us.
But it doesn’t decide where we go.
The waiting List

Raising a Child with Type 1 –
There’s a particular kind of waiting that comes with a chronic condition.
It isn’t passive.
It isn’t optional.
And it isn’t always fair.
It’s the waiting for technology.
The waiting for approvals.
The waiting for funding.
The waiting for a system to catch up with your child’s daily reality.
When your child is diagnosed, you quickly learn what exists.
Insulin pumps.
Newer pumps.
Better algorithms.
Closed-loop systems.
Devices that adjust in real time.
You learn what’s possible.
And then you learn what’s accessible.
Those are not always the same thing.
The 12-Month Reality
In the public system, waiting can mean a year.
A year is long when you’re talking about technology.
It’s even longer when you’re talking about a growing child whose body changes month to month.
A year of:
Manual calculations.
Night-time alarms.
Adjustments and corrections.
Careful dosing.
You understand that resources are finite.
You understand there are other families waiting too.
You understand policy.
But understanding doesn’t shorten the year.
The Quiet Comparison
It’s impossible not to notice what others have access to.
Some children are started on pumps quickly.
Some have private health cover.
Some trial the newest devices early.
And you learn to hold two truths at once:
Gratitude for what you do have.
And awareness of what would help.
There’s no bitterness in it.
Just reality.
The Invisible Cost
The cost of chronic isn’t only financial.
It’s time.
Energy.
Sleep.
Admin.
Phone calls.
Script renewals.
Pharmacy visits.
Supply tracking.
It’s the mental inventory of:
“How many sensors left?”
“When does that script expire?”
“Will this last until the next appointment?”
You become efficient.
Organised.
Prepared.
You don’t have a choice.
Staying Steady in the Waiting
Waiting doesn’t mean doing nothing.
We adjust ratios.
We review patterns.
We treat lows.
We correct highs.
We learn.
She continues growing.
Laughing.
Playing netball.
Going to school.
Being a kid.
Life isn’t paused because the system is slow.
It just requires more of us in the meantime.
Hope, Held Carefully
There will be better technology.
There will be improved access.
There will, one day, be something closer to a cure.
I hold that hope carefully.
Not urgently.
Not desperately.
Just steadily.
Because while we wait for systems to evolve, we keep living.
And while we wait for approvals, we keep packing the school bag.
And while we wait for the next advance, she keeps growing.
A year feels long when you’re looking forward.
But when I look back, what I see isn’t the wait.
I see her resilience.
And that makes it easier to stand in the space between what is available…
And what will be.
Food Isn't just Food Anymore

Raising a Child with Type 1
Before Type 1 diabetes, food was simple.
It was hunger and fullness.
It was growing bodies and busy afternoons.
It was pasta because we felt like pasta.
It was strawberries in a bowl without a calculator beside them.
Now, food is maths.
It’s decisions.
It’s timing.
It’s insulin units and correction factors and carb ratios.
It’s no longer just nourishment.
It’s management.
The Mental Arithmetic
Every meal holds a quiet calculation.
How many carbs in this?
Did we measure properly?
Was that half a cup or closer to three quarters?
Will sport change the outcome?
Is she slightly high already?
Will she spike?
You can learn the numbers.
You can memorise the carb content of strawberries, pasta, milk, chocolate powder.
But what you can’t measure as easily is the emotional weight attached to them.
When Eating Feels Like Effort
For a child with Type 1, eating means insulin.
Every time.
It means:
Planning.
Pausing.
Checking.
Injecting.
Waiting.
Sometimes I wonder if other children realise how effortless their eating is.
They just… eat.
There are days when she says she doesn’t feel hungry at school.
And I hear the layer underneath that.
Because skipping food means skipping insulin.
And skipping insulin feels like skipping the work.
But food isn’t optional.
Not for growth.
Not for energy.
Not for a young girl whose body is still becoming itself.
So we talk gently.
We don’t make food the enemy.
We don’t make numbers the hero.
We try to keep the middle steady.
The Fear No One Prepares You For
There’s a quiet fear that creeps in as they grow older.
Control.
Who controls the numbers?
Who controls the insulin?
Who controls the decision to eat or not eat?
You want to build independence.
But not at the expense of nourishment.
You want her to trust her body.
Even when her body requires intervention.
That balance is delicate.
And constant.
Keeping Food Safe Again
So we try to make food normal.
We cook meals we love.
We measure without making it dramatic.
We correct without blaming.
We treat lows without panic.
We remind her:
Food is fuel.
Food is joy.
Food is not a mistake.
And we protect her relationship with it fiercely.
Because diabetes already takes so much.
It doesn’t get to take food too.
The 2am Club
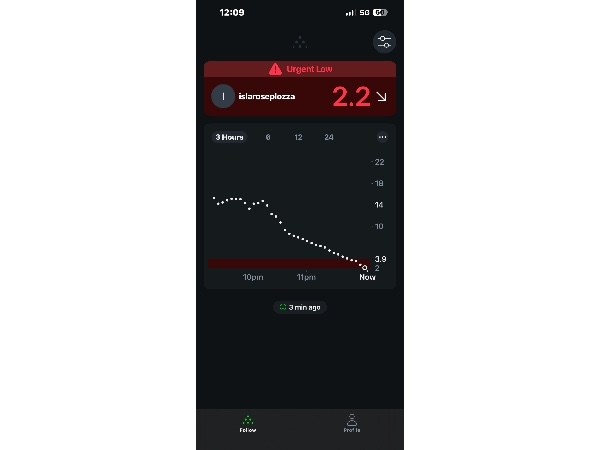
Raising a Child with Type 1 –
There is a version of parenting that happens in the dark.
It’s quiet.
It’s repetitive.
It’s unseen.
And it lives somewhere between 11pm and 3am.
The world sleeps.
Diabetes does not.
The Sound of an Alarm
It doesn’t matter how tired you are.
The alarm cuts through everything.
Not loud in volume — loud in meaning.
Low.
Falling.
Double arrows down.
Or sometimes worse — steady but too low for too long.
Before my feet even hit the floor, my brain is calculating.
How low?
How fast?
Did she have sport today?
Did we give slow-acting carbs before bed?
Did I miss something?
I don’t wake fully.
I switch on.
The Walk Down The Hall
There’s something about that walk.
The house is dark.
The dog is asleep.
The clock ticks.
I open her door softly.
She’s asleep.
Peaceful.
Completely unaware of the invisible maths happening beside her bed.
I recheck the numbers.
I decide:
Glucose tabs?
Juice?
Milk?
Wait and watch?
You learn that treating a 4.8 at 2am is different to treating a 2.9.
You learn that overshooting at night means you’ll pay for it at 5am.
You learn patience.
Even when you don’t have the energy for it.
The Arithmetic of Exhaustion
People talk about being tired with babies.
But no one talks about being tired with a child who has a functioning bedtime routine and a non-functioning pancreas.
Because she sleeps.
But I don’t fully.
Not deeply.
Not without listening.
There’s a layer of vigilance that never switches off.
A mother’s version of background monitoring.
Always humming.
The Fear We Don’t Name
Night-time lows carry a different weight.
Daytime has noise.
Teachers.
Friends.
Movement.
Night-time is still.
And stillness can be frightening.
So, I stay steady.
Measured.
Practical.
I treat the number in front of me.
Not the fear in my head.
Morning Comes Anyway
By morning, she wakes bright.
Stretching.
Asking what’s for breakfast.
Talking about the in day in front.
And I’m calculating how much sleep I actually got.
Sometimes it’s fine.
Sometimes it’s fractured.
But it’s ours.
This is the version of parenting that happens quietly.
No applause.
No audience.
Just numbers in the dark and love strong enough to keep walking down the hallway.
Again.
And again.
And again.
The School Bag

Raising a Child with Type 1 –
There is a moment every morning.
Shoes on.
Hair brushed.
Lunch packed.
And then there’s the bag.
Not just a school bag.
A medical kit disguised as a school bag.
Inside it isn’t just homework and a pencil case.
It’s insulin.
It’s technology.
It’s backup technology.
It’s sugar for emergencies.
It’s the responsibility of staying alive between 9am and 3pm.
And she carries it like it’s normal.
What’s In The Bag
In her bag today:
- Rapid-acting insulin
- Backup pen needles
- Glucose meter
- Test strips
- Hypo treatments
- Spare snacks
- CGM receiver
- Emergency glucagon
- Written care plan
- Extra “just in case” supplies
Most kids carry a jumper they’ll never wear.
Mine carries contingency plans.
The Quiet Letting Go
When she walks through the school gates, there’s a physical letting go.
But there’s also a mental one.
I’m not there when she lines up for sport.
I’m not there when she decides whether to eat everything in her lunchbox.
I’m not there if she feels her blood sugar dropping in the middle of class.
She is.
At what age does a child become responsible for monitoring their own pancreas?
Because that’s what this is.
We call it “independence.”
But sometimes, it feels like acceleration.
The Questions I Don’t Always Ask
Did you bolus?
Did you correct?
Did you check before netball?
Did you feel low?
Did you treat it properly?
If I ask too much, she feels watched.
If I don’t ask enough, I feel negligent.
So, I walk the middle line.
Calm. Casual. Steady.
“How was your day?”
And meanwhile I’m scanning graphs.
The Invisible Pressure
There’s something heavy about sending your child out into the world with medical equipment in her bag.
Not because she’s incapable.
But because she shouldn’t have to be.
She should just be thinking about:
- Friends.
- Homework.
- Who’s playing centre in netball.
- What book she’s reading.
Instead, she’s also thinking:
Am I high?
Am I low?
Do I need insulin?
Should I wait?
That’s a lot for a young mind.
Even when she handles it beautifully.
What Strength Looks Like
Strength doesn’t always look loud.
Sometimes it looks like an 12-year-old girl pulling a juice popper out of her bag without making a fuss.
Sometimes it looks like checking her numbers discreetly, so she doesn’t feel “different.”
Sometimes it looks like telling me she’s fine, even when she’s tired of it all.
The school bag sits by the door every afternoon when she comes home.
Unzipped.
Relieved.
Another day navigated.
Another day managed.
Another day she carried more than most people will ever realise.
And tomorrow?
We’ll pack it again.
The Supplies you never see
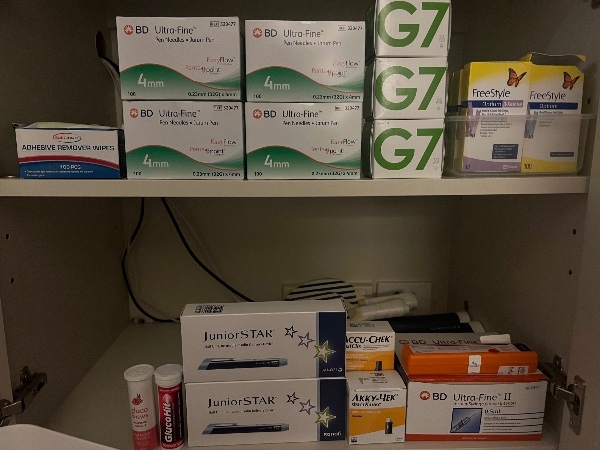
Raising a Child with Type 1
When people hear “Type 1 diabetes,” they usually think of one thing.
Insulin.
They don’t picture the drawer.
Or the backup drawer.
Or the pouch inside the school bag.
Or the spare kit in the car.
Or the emergency stash in my handbag.
If I hadn’t worked in pharmaceuticals before becoming a mum navigating this, I think it would have completely overwhelmed me. Even with that background, there are days it still does.
Because Type 1 isn’t just a condition.
It’s logistics.
It’s preparation.
It’s never walking out the front door casually again.
What One Child Actually Needs
Here’s what our “normal” requires:
Insulin
Rapid-acting insulin for meals and corrections.
Long-acting insulin (if injections are needed).
Delivery devices
Insulin pens.
Pen needles.
An insulin pump.
Pump pods or infusion sets.
Spare cannulas.
Backup pens in case technology fails.
Glucose monitoring
Continuous Glucose Monitor (CGM).
Sensors.
Transmitter.
Overpatches.
Alcohol wipes.
Charging cables.
Backup testing
Glucose meter.
Test strips.
Lancets.
Finger pricker.
Hypos (low blood sugar)
Glucose tablets.
Juice poppers.
Jellybeans.
Emergency glucagon injection.
Highs (ketone risk)
Blood ketone strips.
Extra insulin.
Skin & adhesive care
Barrier wipes.
Adhesive remover.
Medical tape.
And that’s before we talk about:
Prescriptions.
PBS limits.
Pharmacy runs.
Camp planning.
School communication.
Heat management in summer.
Double-packing for excursions.
Triple-packing for holidays.
Nothing about this is spontaneous.
Everything is calculated.
The Mental Packing List
Every time we leave the house, I run through the quiet checklist in my mind:
Insulin?
Backup insulin?
Meter?
Strips?
Hypo treatment?
Enough snacks?
Charged receiver?
Emergency plan?
And then — the hardest question —
Is she okay?
Because the supplies are visible.
The numbers are visible.
But the emotional weight isn’t.
The Part No One Sees
People don’t see the 11pm scan of a glucose graph.
They don’t see the pause before sport.
They don’t see a child calculating whether she’s “high enough” to play safely.
They don’t see the tiny negotiations happening in her head around food.
They don’t see the way I ask, “Are you okay?” more than any child should have to hear.
Type 1 diabetes is a condition of preparation.
Preparation for lows.
Preparation for highs.
Preparation for what if.
What I’m Grateful For
I’m grateful I understand medications.
I’m grateful I know how dosing works.
I’m grateful medical language doesn’t scare me.
But I shouldn’t have to.
No parent should need a pharmaceutical background to feel steady in this.
What steadies me isn’t the training.
It’s her.
Her resilience.
Her ability to still be a kid.
Her netball games.
Her laughter.
Her stubborn independence.
The real strength isn’t in the kit.
It’s in the kid.
The Day Everything Changed
Raising a Child with Type 1
There is a before. And there is an after.
Before Type 1 diabetes, she was tired. Thirsty. Going to the bathroom more than usual. The subtle loss of weight.
We noticed, but not in a way that felt urgent.
Children get tired. Nothing prepares you for the moment someone says the words:
“It’s Type 1 diabetes.” The Word “Chronic “You don’t hear the rest immediately.
You hear:
Autoimmune.
Insulin.
Hospital.
Lifelong.
And then your brain narrows its focus to one single truth: Her pancreas has stopped working. There is no tablet to restart it. It is not a phase to grow out of. This is forever.
The Room Doesn’t Spin
People talk about the world tilting in moments like this. For me, it didn’t tilt It sharpened.
I went practical.
Questions.
Dosing.
Next steps.
What do we do now?
Working in pharmaceuticals meant medical language didn’t frighten me. Insulin didn’t feel mysterious. Protocols made sense. And I am deeply aware that this helped steady me in those first hours. Because without that background, I think the flood of information would have been completely overwhelming. Even with it — it was a lot.
Watching Her Learn It
What I remember most is not the monitors. Not the education sessions. Not the injection training. It’s her face. Listening. Trying to understand. Holding back her tears.
Brave in that way children sometimes are when they don’t yet fully grasp the weight of what they’re being told. We were learning how to keep her alive. And she was learning that her body had changed. That’s a lot for anyone. Let alone a child.
The First Injection
The first insulin dose changes something. It’s the line between before and after.
Before, her body handled this silently. After, we step in. Manually. Deliberately. Every day. You don’t celebrate the first injection. But you remember it.
What I Know Now
I know now that diagnosis isn’t the hardest part.
It’s the beginning.
The days and nights after.
The 2am alarms.
The school bag.
The food calculations.
The waiting lists.
The explanations.
Those are the rhythm of it.
But diagnosis is the doorway.
The moment your family quietly shifts into a new version of normal.
What Stayed the Same
Here is what didn’t change:
She is still her.
She still laughs loudly.
She still plays netball.
She still piles clothes on her floor.
She still rolls her eyes at us when we ask too many questions.
Diabetes arrived.
But it didn’t replace her.
It just became something we carry alongside everything else.
There is a before.
And there is an after.
But there is also a through.
And we are walking it.
Together.
Rebecca 🤍
I'm walking for a world without type 1 diabetes in Geelong!
I'm joining the world's largest type 1 diabetes (T1D) fundraising event for families at Barwon Valley Park this March!
Why? To help raise $1.1 million for life-changing T1D research, and ultimately turn type 1 into type NONE.
T1D can strike anyone at any time, and 8 Australians are diagnosed with it every day. Diagnosis means a 24/7 fight with no break, and facing an extra 180 decisions a day to remain safe and healthy.
Please support my walk today.
My One Walk fundraising achievements

Set profile picture

Donated to self

Shared Page

Reached Fundraising Target



Power Walker

Athlete

Elite Walker

Increased Fundraising Target Over $500
Thank you to my Sponsors

$263.75
Corin Warhurst

$263.75
Mohammed And Samantha Daghistani
Love you Isla!

$263.75
Patti Spicer

$263.75
Paul Plozza

$263.75
Laura, Mazie And Poppy
Love you Bec! You got this!

$263.75
Peter Plozza/lee Edge
Your a champion

$200
Michelle Plozza
Go Team Becci!

$200
Pat Steuten
Great job Becci 🩷

$154.65
Tess & Patrick
Great job Bec x

$131.88
Al
Thinking of you with all that you are carrying today x

$131.88
Sue Laughton
Here’s hope for the ongoing research leading to a better treatment.

$131.88
Allison Wisby
❤️

$131.88
Mim And Az
The journey and responsibility is huge. People totally underestimate this disease. Managing it along with advocating for research and funds can be exhausting. Always here if you need.

$125
Brooke Froud-cummins
💜💜💜

$106.12
Mark Spicer
Happy to chip in Becci

$100
Sarah Moorhouse
💖

$54.12
Sarah Lake

$54.12
Handley Family

$54.12
Rach Cash
💕

$54.12
Belinda Emmett
🩵

$54.12
Anonymous

$54.12
Meg Dooley

$54.12
The Keenan Family
We're proud to support your walk for a world without type 1 diabetes.

$54.12
Susan Sadler
Go girl! 💪

$54.12
Adriana
Lovely Bec, you are amazing and I admire you so much. Good luck doing the walk my friend. Lets hope the cure will be found very soon xxx

$54.12
Sue Wall

$54.12
Tuan Diep

$54.12
Angeline Mclaughlin
Cheering you on every step of the way.

$54.12
Carly Enticott
Amazing effort and fabulous cause x

$27.81
Anonymous

$27.81
Merril

$27.81
Susan Priest
Good luck Rebecca! You’re amazing Isla!

$27.21
Kelly Fleischer
Great work Bec! 💕

$25
Loraine Richards
Good luck Becs on the walk. Xx

$14.98